Alexander Heights
Ph (08) 9343 0278 or 0422 710 020
"Awarded for
Excellence in Optometry
by Avenue Perth
(2024-2026)"
OPENING HOURS
Mon – Fri: 10 am – 5 pm
Sat: 10 am – 4 pm (some: 10 am – 1 pm)
Sun & Public Holidays: Closed
Other times: By appointment

Urgent Eyecare / Emergency / Eye Injury
Our experienced therapeutic optometrist has the expertise to diagnose and manage eye emergency conditions accurately and efficiently, such as foreign bodies, eye pain, red eyes, headaches, retinal and macular emergency. Our practice is very well equipped to handle eye emergency conditions. For example, high resolution magnified photography and scans of both external and internal eye health is available to show and explain to patients for fully understanding of their conditions to improve their compliance of treatments for effective management. For those eye emergency conditions required to be managed by ophthalmologists or other medical professionals, emergency referrals and appointments can be arranged swiftly.
Our optometrist worked in an eye specialist clinic in a hospital. He is a certified and registered as therapeutic endorsed optometrists in Australia, therefore, he is able to prescribe many eye medications to treat common eye conditions.
Some of the emergency cases have been diagnosed and managed are as below:
Removal of Embedded Corneal Foreign Body
A corneal foreign body is one of the main causes of blindness. The effects can range from mild infections (corneal abrasion, keratitis) to severe damage (endophthalmitis) depending on the type of material. Late-stage complications can cause permanent blindness. (Reference: The Influence of Corneal Foreign Body on Eye Infection | Atlantis Press (atlantis-press.com)
.jpg)
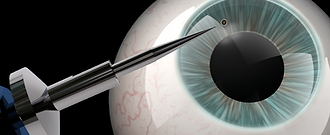
Patient: 74 year old man came in with foreign body sensation with blinkings in his right eye. Normal vision was reported.
History: A metal foreign body was found embedded in his nasal peripheral cornea outside the pupillary zone.
Examination: High resolution magnified images were taken and used for explaining the conditions and procedures required to the prepare the patient psychologically in order to avoid panic attack; and documenting the conditions and severity for future reference and comparision.
Management: After his consent of proceeding the procedure, local anesthetic eye drops were applied and the foreign body was gently and painlessly removed with a sterilized tool. Rust residues and stain were found underneath and then successfully removed by another sterilized special tool without any discomfort.
Eye medication and instructions were given, and a review in 24 hours was scheduled to ensure normal wound healing without any complications.
#3415
Guide: Local experienced therapeutic optometrists with sufficient equipment and tools, such as slit lamp imaging and foreign body removal tools, including corneal rust ring remover Algerbrush, are the best practitioners to manage these cases. All cases should return in 24 hours (or sooner if symptoms worsen) for re-evaluation to ensure the corneal wound healing normally. Untreated corneal infection and ulcers can lead to severe permanent vision loss and even loss of an eye. Close follow-up until the corneal epithelial defect resolves.
Emergency Case: Severe Central Corneal Abrasion

Patient: Female, early 40's (AH3824)
Symptoms: Left eye with severe pain with blurry vision after removing her disposable soft contact lens.
Signs: Severe central corneal abrasion involving pupillary zone.
Management: Lay-off contact lens. Prescription (non over-the-counter) antibiotic eye drops for contact lens wearer were prescribed. Refer to see an ophthalmologist urgently. A few visits were required to monitor the progress.
Outcome: Cornea healed gradually over weeks and vision was still affected. Spectacle prescription changed and new lenses were required.
Guide: Many contact lens wearers, especially disposable lenses, have poor compliance or even ignore hygiene, source of lenses and solution (if any), regular lens replacements and checkup schedules. In fact, they are exposing themselves to the risks of permanent severe visual impairement. Contact lens wear is very safe if professional instructions and ongoing
guidance and are followed. However, updated
information and guidance cannot be obtained from the practitioners if checkups are ignored or avoided. In fact, any eye problems arised might
cause pain, inconvenience, substantial cost to manage and treat them. In some cases, visual impairment can affect their independence, life style, job, income and future. Simply following professional advice is the best way to avoid all these issues.
Emergency Case: Bleeding Inside The Eyeball & High Eye Pressure After Hit By A Soccer Ball
Patient: Male, mid-teen (AH1746)
Symptoms: Blurry vision, foreign body sensation, no pain.
Signs: Bleeding reaching the bottom of vertically distorted pupil in the anterior chamber; high eye pressure reaching acute glaucomatous level.
Management: Refer to see an ophthalmologist very urgently. This case usually requires at least a few visits to manage for these two complicated conditions. He might need eye surgeries and life-long management.
Guide: Many people do not any wear protective eyewears for sports. This case really demonstrated their importance and showed the potential consequence of ignoring professional advice. Our eyes are extremely delicate and also extremely important for seeing. We need good eye health for good vision to function, drive, learn, work, earn our living now or future and enjoy life; all of these will be affected or lost without with proper eye protection. Some jobs require good vision of both eyes. From my experience, most people either don't know or ignore sufficient eye protection; and they are taking high level of risk which can be easily prevented.


